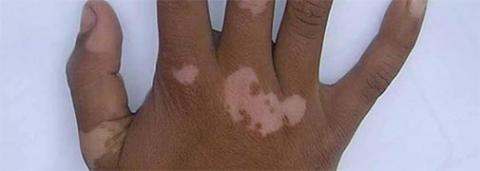
Vitiligo affects between 0.1-2% of the population. Some recent studies have calculated the incidence among Italian males to be 0.17 and among Indians 1.84%. In 50% of the patients, vitiligo onsets before the age of 18. It can occur at any age but usually peaks between ages 10-30.
There have been cases of vitiligo occuring even after the age of 50. Everyone can get vitligo, there are no racial, ethnic or socioeconomic associations. Vitiligo patients can be diagnosed with two variations of the disease:
- segmental
- nonsegmental vitiligo
Segmental vitiligo usualy appears on one side of the body (unilateral involvement), has an early onset and rapid progression. This type of vitiligo is most likely linked to neurological disorders. Nonsegmental vitiligo represents 72-95% of the vitiligo cases. It is usually symetric and new patches appear throughtout one's life. This type of the vitiligo has most likely autoimune origins.
Risk Factors
20-30% of vitiligo patients have a first or second-degree relative with the diesease. Another risk factor is represented by a stressful life event in the last 12 months. Vitligo onset may be triggered by other events such as pregnancy, sunburn or skin trauma.
Sometimes, vitiligo is asociated with a couple of other autoimune disorders such as:
- Hashimoto's thyroiditis
- Grave's disease
- diabetes mellitus
- Addison's disease
- alopecia areata
- pernicious anemia
- rheumatoid arthritis
- autoimmune polyglandular syndrome
- psoriasis
Diagnosis
A woods lamp examination can detect the absence or presence of pigment. Bright white or blue, under this light can indicate depigmentation.
The course of disease is unpredictable. Lesions may be stable, progress slowly or rapidly cause complete depigmentation within 1-2 years.
Treatment
Once the disease has been properly diagnosed, the treatment can consist of:
Topical medications
- corticosteroids
- tactolimus 0.1%
Oral medications
- Ginko biloba
Phototerapy:
- nbUVB is the most efective type of therapy available.
- pUVA - psoralen + UVA may have a positive outcome
Surgical therapy:
May be the solution for localized vitiligo that is resistant to other medical interventions. The surgical therapy can consist of autologous transplanted epidermal cell suspension or epidermal blister grafting.